Why Digital Radiography CE Matters for Your Career and Patient Safety
Digital radiography ce is continuing education on modern X-ray technologies like Computed Radiography (CR) and Direct Radiography (DR). Radiologic technologists must complete these courses to maintain licensure and stay current with evolving imaging standards.
Quick Answer for Your CE Requirements:
- ARRT requires 24 Category A CE credits every two years (biennium)
- California mandates at least 4 of those 24 credits specifically in digital radiography
- Most states accept ASRT-approved courses that cover CR/DR fundamentals, radiation safety, and image quality
- You need to understand exposure indicators, dose creep prevention, and proper collimation techniques
- Courses typically cover digital image processing, PACS integration, artifact management, and radiation protection
The shift from film to digital has created new challenges. Digital systems can mask exposure errors, leading to a phenomenon called dose creep, where patients may receive radiation doses three to five times higher than necessary without any visible image degradation. This makes proper training essential.
Many experts note that technologists trained on analog systems have a strong foundational understanding of exposure principles, a skill that is critical in the digital age.
Whether you’re a Certified Radiologic Technologist (CRT) renewing your California license or an ARRT registrant fulfilling biennium requirements, understanding CE can be confusing. State rules vary, and not all courses satisfy mandatory credits.
This guide cuts through the confusion to help you find high-quality, accredited digital radiography CE that meets your state requirements, fits your schedule, and improves your clinical practice.
Understanding the Core Concepts of Digital Radiography
To meet your digital radiography ce requirements, you need to understand how modern X-ray imaging works. Digital radiography is a fundamentally different way of capturing, processing, and viewing images, revolving around image capture methods, image processing, and workflow speed. Both Computed Radiography (CR) and Direct Radiography (DR) convert X-ray energy into digital data for manipulation and storage in a Picture Archiving and Communication System (PACS).
The difference between CR and DR directly impacts workflow, patient throughput, and image quality. Here’s how they compare:
| Feature | Computed Radiography (CR) | Direct Radiography (DR) |
|---|---|---|
| Image Capture Medium | Photostimulable Phosphor (PSP) plate | Flat-panel detector (direct or indirect conversion) |
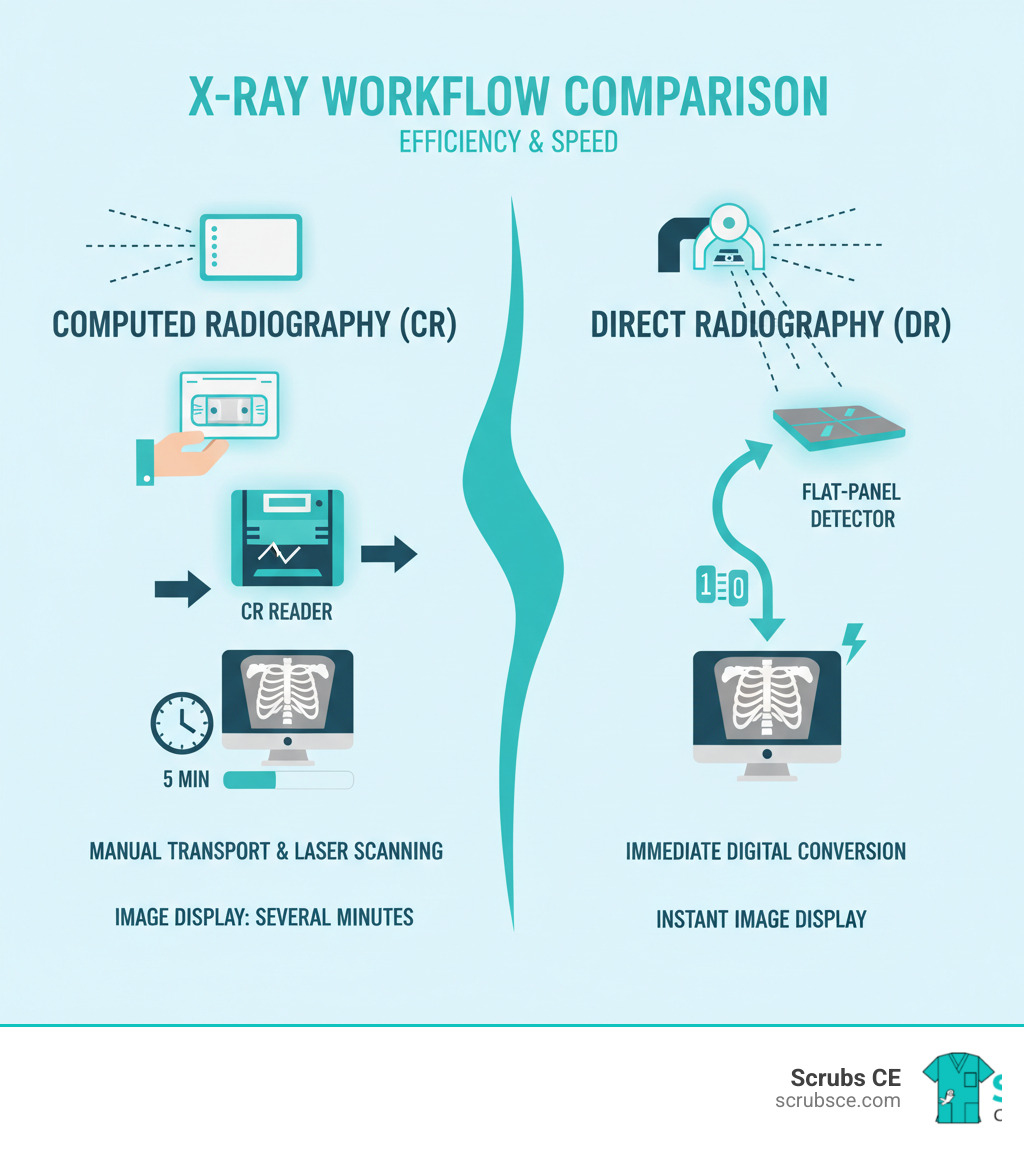
| Workflow Steps | Expose plate → Process in CR reader → Image displayed | Expose detector → Image displayed instantly |
| Image Availability | Minutes (requires plate processing) | Seconds (immediate) |
| Image Quality/Resolution | Good, but generally lower than DR | Excellent, higher spatial resolution and contrast |
| Initial Cost | Lower (can use existing X-ray units) | Higher (integrated system) |
Understanding these differences helps explain why some facilities use CR (budget constraints) while others choose DR (high patient volume, need for speed).
The Shift from Film to Digital
The transition from film to digital eliminated the darkroom and transformed radiographic practice. Post-processing capabilities allow for adjustments to brightness, contrast, and magnification after the exposure, often salvaging a suboptimal technique and reducing repeat exposures.
This flexibility contributes to reduced patient dose potential. Digital receptors are more sensitive than film, allowing for diagnostic images with lower radiation settings and upholding the ALARA principle (As Low As Reasonably Achievable). Furthermore, digital imaging simplifies data storage and archiving in PACS, eliminating physical film libraries and reducing technical issues like chemical streaks or processor artifacts.
However, digital’s forgiving nature can mask poor technique, which is why quality digital radiography ce is so important. To strengthen your foundational knowledge, see our A Guide to Continuing Education for X-Ray Technologists.
How CR and DR Systems Work
Computed Radiography (CR) acts as a bridge between film and fully digital systems. It uses a Photostimulable Phosphor (PSP) plate in a cassette to capture a latent image. The cassette is taken to a CR reader, where a laser scanning system stimulates the plate, causing it to release light. A photodetector converts this light into a digital signal. The plate is then erased and ready for reuse.
Direct Radiography (DR) eliminates the reader step by using flat-panel detectors. These detectors work in one of two ways:
- Indirect conversion uses a scintillator to convert X-rays into light, which is then converted into an electrical charge and digitized.
- Direct conversion detectors convert X-ray photons directly into an electrical charge, which is then digitized.
The main advantage of DR is immediate image display, which dramatically improves workflow in busy departments. To learn more about these systems, our course Radiography in the Digital Age 3rd Ed covers these principles in detail.
Mastering Image Quality and Radiation Safety
Digital radiography’s flexibility is a great asset, but it requires vigilance to maintain image quality and protect patients from unnecessary radiation. Upholding the ALARA principle (As Low As Reasonably Achievable) is the ethical foundation of our profession. Every exposure must achieve a diagnostic image with the minimum necessary dose. This involves preventing artifacts, implementing quality control, and ensuring both patient and staff safety.
Managing Radiation Dose: Exposure Indicators and Dose Creep
Unlike film, which provides immediate visual feedback on exposure, digital systems rely on Exposure Indicators (EI). These are numerical values (e.g., Fuji’s S-number, Carestream’s exposure index) that report the amount of radiation that reached the receptor. It is critical to understand your facility’s target EI ranges to ensure appropriate dosage. For more information, see resources like Watch Exposure Indicators.
This reliance on numerical indicators is necessary because digital systems can lead to dose creep—the gradual, unintentional increase in radiation exposure over time. Digital detectors have a wide exposure latitude and can produce acceptable-looking images even when significantly overexposed. With film, overexposure created a dark, unusable image. With digital, post-processing can mask the error, but the patient still receives an unnecessarily high dose.
This risk grows when technologists use higher techniques “just to be safe.” Without diligent monitoring of EIs, patient doses can become three to five times higher than necessary. Preventing dose creep requires discipline: review EIs for every image, adhere to technique charts, and take digital radiography ce that reinforces these best practices. Our Radiographic Imaging and Exposure 5th Ed Ebook Test digs deep into exposure management.
The Critical Role of Collimation and Artifact Management
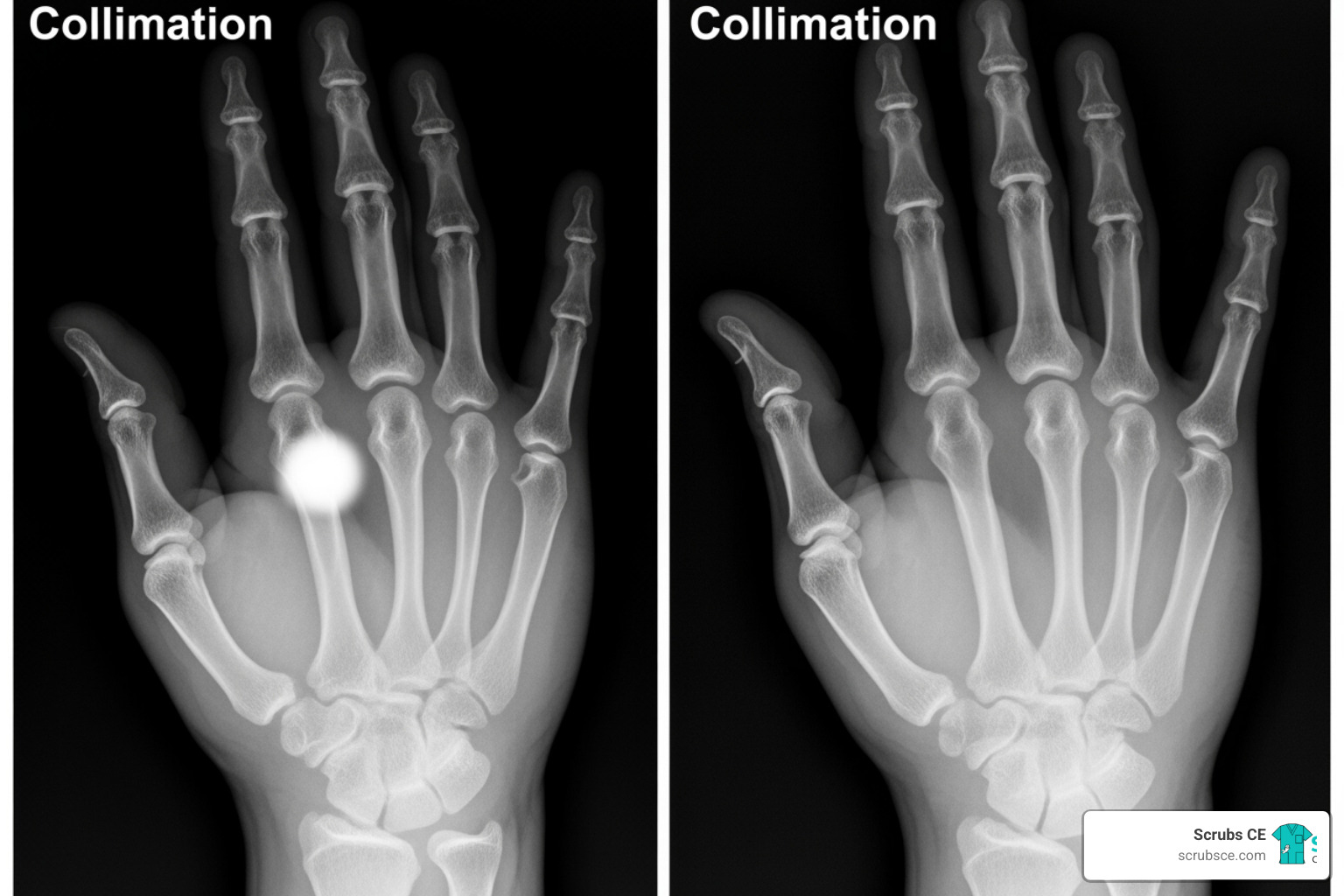
Physical collimation—restricting the X-ray beam to the area of interest—is a fundamental skill with a powerful impact. Proper collimation reduces patient dose and improves image quality by minimizing scatter radiation, which degrades contrast and detail.
It is crucial not to confuse this with electronic masking (or shuttering). This post-processing tool digitally crops an image to make it look properly collimated, but it does nothing to reduce the patient’s radiation dose or prevent the scatter that already occurred. Real collimation happens before the exposure. For examples, see Collimate to improve image quality.
Technologists must also be able to identify image artifacts. Common digital artifacts include:
- Plate reader artifacts (CR): Caused by dirt, laser issues, or transport problems.
- Dead pixels (DR): Non-functioning detector elements that appear as dots.
- Image noise: A grainy appearance, often from low mAs (quantum mottle) or electronic interference.
- Uberschwinger: A halo effect around metal implants from excessive edge improvement.
- Lag or ghost images: Residual signals from previous exposures.
Understanding these artifacts is essential for troubleshooting. Quality digital radiography ce courses like Radiographic Image Analysis help you develop the critical eye needed to spot and correct these issues.
Navigating Your Digital Radiography CE Requirements
Keeping your credentials current means navigating a maze of CE requirements from national and state boards. While it can seem complex, quality digital radiography ce courses are often designed to satisfy these overlapping demands with Category A credits.
ARRT and State-Specific Digital Radiography CE Mandates
The American Registry of Radiologic Technologists (ARRT) sets the baseline, requiring 24 Category A CE credits every two years (a biennium). However, state licensing boards often add their own specific mandates.
California is a key example. The Radiologic Health Branch (RHB) requires Certified Radiologic Technologists (CRTs) to complete 24 approved CE credits every two years, with a crucial stipulation: at least 4 of those 24 credits must specifically cover digital radiography. This rule also applies to Limited Permit X-Ray Technicians (XTs) with digital authorization. You can verify this on the California Department of Public Health – Radiologic Health Branch (RHB) Continuing Education Requirements page.
Other states like Florida and Texas have their own distinct requirements. Always check with your specific state licensing authority to confirm their expectations. Our guide on How Many X-Ray CE Credits Do I Need for Radiography? can help break down these variations.
Finding Approved Digital Radiography CE Courses
To ensure your courses count, look for proper accreditation. ASRT approval is the gold standard, as these courses are accepted by the ARRT for Category A credit and by most state boards.
Beyond accreditation, choose courses that cover the material you need for both professional development and state mandates. The best digital radiography ce programs address these core areas:
- Fundamentals of CR/DR Systems
- Radiation Safety and Dose Reduction
- Digital Image Processing and Artifacts
- PACS and Healthcare Informatics
These topics form the foundation of competent digital practice and will typically satisfy state-specific content requirements. We know finding time for CE is challenging, which is why our Continuing Education Courses for X-Ray Technologists are ASRT-approved, self-paced, and designed to meet both ARRT and state-specific mandates like California’s.
The Future of Digital Radiography and Lifelong Learning
Digital radiography is constantly evolving, which is why lifelong learning is so critical. Digital radiography ce is not just about licensure; it’s about staying relevant in a rapidly changing profession.
The biggest game-changer on the horizon is Artificial Intelligence (AI). AI is already entering imaging suites through machine learning algorithms that can recognize patterns in images that the human eye might miss.
Computer-Aided Diagnosis (CAD) systems are a prime example. These AI tools can flag potential abnormalities and highlight areas for a radiologist’s attention. They are not here to replace us, but to augment our skills. AI is also being used to optimize exposure parameters in real-time and analyze patient positioning to reduce repeats.
This technological shift will evolve our roles. We will need to understand how AI systems work, their limitations, and the ethical considerations surrounding their use in healthcare, such as data privacy and algorithmic bias.
Future digital radiography ce will need to cover AI fundamentals, CAD tool integration, and how to interpret their outputs. The technologists who thrive will be those who accept continuous learning and see these advancements as an opportunity to provide better, safer patient care.
Staying ahead is about being the best possible advocate for our patients. Understanding the latest technologies ensures they are used safely and effectively. As we stand on the edge of radiology’s next great change, The Importance of Continuing Education (CE) for X-Ray Technologists has never been more apparent.
Frequently Asked Questions about Digital Radiography CE
Navigating continuing education requirements can be confusing. Here are clear answers to the most common questions we hear from technologists.
How many digital radiography CE credits do I need?
This depends on your credentials and where you work. The ARRT requires 24 Category A CE credits every two years to maintain your registration. However, many states add their own rules. For example, California requires that at least 4 of those 24 credits be specifically in digital radiography. This applies to both CRTs and XTs with digital authorization. Always check with your specific state licensing board to confirm their requirements. Our guide on What You Need to Know About X-Ray Continuing Education Requirements can help clarify state-by-state rules.
What is ‘dose creep’ and why is it a concern in digital radiography?
Dose creep is the gradual, unintentional increase in radiation exposure to patients over time. It happens because digital detectors have a very wide exposure latitude, meaning they can produce a perfect-looking image even when significantly overexposed. Unlike film, there are no immediate visual cues of overexposure. This creates a risk of patients receiving much higher doses than necessary. The only way to prevent dose creep is by diligently monitoring Exposure Indicators (EI) on every image. Organizations like Image Wisely promote awareness of this critical safety issue.
Can I use the same CE course for my ARRT and state license renewal?
In most cases, yes. A digital radiography ce course that is ASRT-approved for Category A credit will typically be accepted by both the ARRT and your state licensing board. This allows you to satisfy multiple requirements with a single course.
However, you must verify that the course content meets any specific state mandates. For example, a general radiation safety course will count for your ARRT credits, but it may not fulfill California’s mandatory 4-credit requirement for digital radiography content. Always read course descriptions carefully to ensure they align with your state’s rules. Our courses are designed for broad acceptance, including Accepted Everywhere, Guaranteed for ARRT Category A credit, but a final check with your state board is always a good idea.
Conclusion
Digital radiography ce is more than a requirement—it’s a commitment to professional excellence and patient safety. Digital technology has given us incredible tools, but it also brings responsibilities. The same systems that improve efficiency can mask issues like dose creep, where patients receive excessive radiation without any visual warning. Mastering exposure indicators, collimation, and artifact recognition are essential skills for modern practice.
CE requirements, like the ARRT’s 24 credits or California’s 4-credit digital mandate, exist to keep us sharp and engaged with new developments, from PACS integration to emerging AI. Quality continuing education bridges the gap between compliance and professional growth, providing practical knowledge that improves your daily work and patient outcomes.
At ScrubsCE, we build our courses with this in mind. We offer ASRT-approved, state-compliant courses that are self-paced, convenient, and filled with useful content. You get practical skills for your next shift and an instant certificate upon completion.
Whether you’re preparing for the future of AI-assisted imaging or ensuring you meet today’s state requirements, we are here to support your career journey. Continuing education is how we not only keep up but move forward, providing the safest, highest-quality care possible.
Ready to tackle your CE requirements with courses that matter? Browse our full catalog of Radiology CE courses and find what you need to keep your license current and your skills sharp.

Recent Comments