Why Informatics in Radiology Matters More Than Ever
Informatics in Radiology is the subspecialty that applies information technology to improve how medical images are acquired, stored, managed, and interpreted. At its core, it’s about making Radiology more efficient, accurate, and accessible by leveraging digital tools, data systems, and artificial intelligence.
Key aspects of Radiology informatics include:
- Picture Archiving and Communication Systems (PACS) – Digital storage and retrieval of medical images
- Radiology Information Systems (RIS) – Managing patient data, scheduling, and workflow
- DICOM and HL7 Standards – Protocols that enable different systems to communicate
- Artificial Intelligence Applications – Tools that assist radiologists in detecting abnormalities
- Enterprise Imaging – Integrating imaging data across entire healthcare organizations
The field has evolved dramatically from film-based X-rays in physical libraries to cloud-based systems where images can be accessed instantly from anywhere. As one journal article puts it, Radiology is “an inherently data-intensive and technology-driven specialty” that depends on robust informatics infrastructure to function.
The impact is significant. For example, AI-assisted CT reading can reduce radiologist reading time by more than 44% for certain findings. Even small efficiency gains add up—cutting just 12 seconds per case allows a radiologist reading chest X-rays every 2 minutes to get home an hour earlier during a 10-hour day.
I’m Zita Ewert, and through my work at SCRUBS Continuing Education, I’ve seen how critical informatics in Radiology has become for imaging professionals seeking to stay current with evolving technology and maintain their certifications. My focus is on making complex topics like imaging informatics accessible through practical, regulatory-compliant continuing education.
The Core Components of Informatics in Radiology
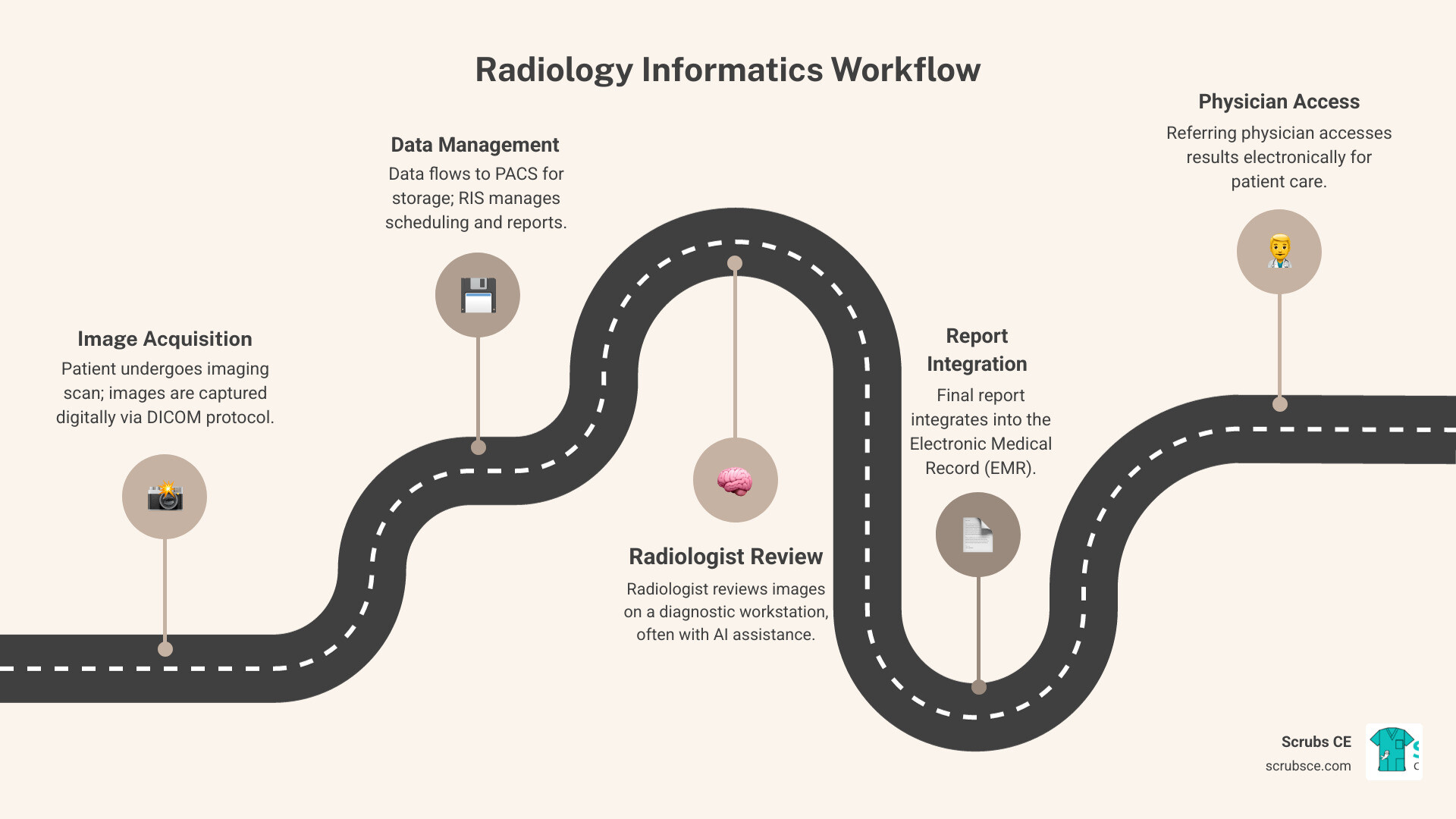
At the heart of modern Radiology lies a sophisticated network of interconnected systems, working in harmony to manage the vast amounts of data generated by medical imaging. These core components are what make informatics in Radiology a mission-critical function in healthcare today.
Picture Archiving and Communication Systems (PACS)
Think of PACS as the digital library for all medical images. Before PACS, Radiology departments relied on physical film stored in massive warehouses. With PACS, digital images—from X-rays, CTs, and MRIs—are instantly captured, stored, and made available. A typical PACS includes imaging modalities, a secure network database, high-resolution viewing workstations, and long-term archiving solutions.
The FDA even reclassified PACS in 2021 to a Medical Image Management and Processing System (MIMPS), reflecting its evolving role. Essentially, PACS allows for secure storage and transmission of digital images, facilitating quick transfers with patient names, diagnoses, and other critical information.
Radiology Information System (RIS)
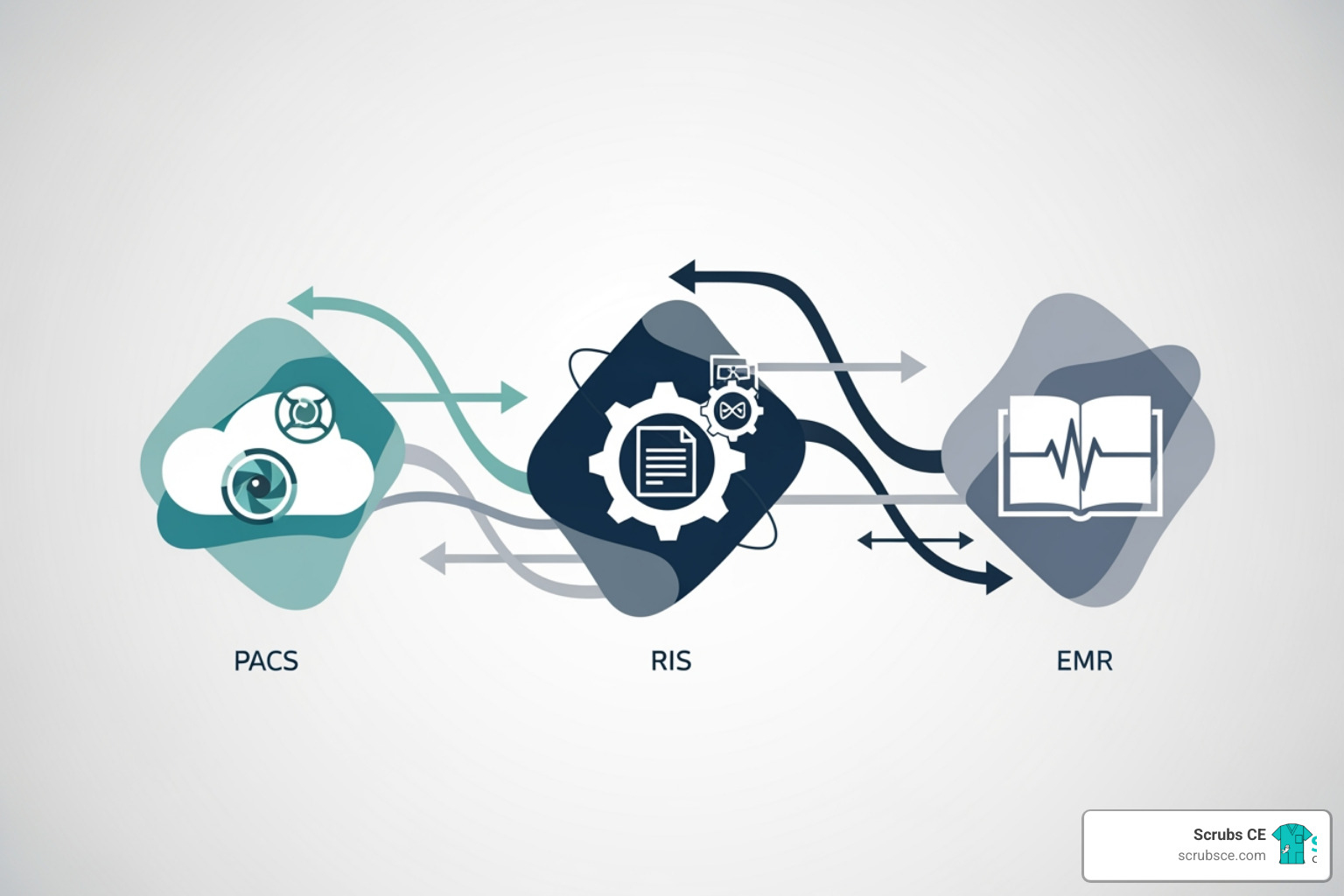
While PACS handles the images, the Radiology Information System (RIS) manages the workflow and administrative data. It’s a specialized database that helps professionals track patient data and files, streamlining operations. A RIS typically handles patient registration, scheduling, patient flow management, and reporting, often integrating with PACS and EMRs.
Electronic Medical Record (EMR)
The Electronic Medical Record (EMR) is the overarching digital record of a patient’s health information. Informatics in Radiology plays a crucial role by ensuring seamless data sharing between PACS/RIS and the EMR. This allows referring physicians to access Radiology reports and images directly from the patient’s comprehensive medical chart, which is vital for coordinated care.
Vendor Neutral Archive (VNA) and Workflow Orchestration
Many modern healthcare systems also employ a Vendor Neutral Archive (VNA), a universal storage solution for all imaging data, regardless of the vendor. This is key for enterprise imaging, which aims to integrate all images (Radiology, cardiology, pathology, etc.) into a single platform. This helps avoid vendor lock-in and simplifies data migration.
Together, these systems facilitate intricate workflow orchestration, ensuring each step from order to final report is managed efficiently. For a deeper dive into these components, we recommend exploring “A Review of Core Concepts of Imaging Informatics.”
How Standards like DICOM and HL7 Enable Connectivity
The magic behind these interconnected systems is their ability to “speak the same language.” This is where imaging informatics standards come into play, facilitating interoperability—the ability of different systems to access, exchange, and use data in a coordinated manner.
Digital Imaging and Communications in Medicine (DICOM)
DICOM is the universal language for medical images and related information. Developed by the American College of Radiology (ACR) and the National Electrical Manufacturers Association (NEMA), DICOM defines image formatting, communication protocols, and how metadata (patient info, study details) is embedded in the image file. As the “Basics of Imaging Informatics: Part 1” article explains, DICOM rules allow digital imaging studies to move between disparate systems. However, some proprietary subfields in DICOM can still create challenges, as highlighted in “Digital mammography, networking, PACS, and Dante’s Inferno,” underscoring the ongoing need for universal standards.
Health Level Seven (HL7)
While DICOM focuses on images, Health Level Seven (HL7) is the primary standard for exchanging general healthcare information, such as patient admissions, lab results, and Radiology orders. It’s crucial for connecting Radiology departments with the broader hospital information system (HIS) and EMR.
Integrating the Healthcare Enterprise (IHE)
Building on DICOM and HL7, Integrating the Healthcare Enterprise (IHE) creates profiles that define how systems should use these standards to address specific clinical needs, providing practical guidance for vendors and purchasers.
The Evolution of Imaging Informatics
The journey of informatics in Radiology is a story of innovation driven by the pursuit of better patient care.
It began in 1895 with Wilhelm Conrad Röntgen’s findy of X-rays. For decades, Radiology was synonymous with film, a slow and inefficient process. The development of CT in the 1970s and MRI in the 1980s generated an unprecedented volume of images, overwhelming film-based systems.
This data deluge necessitated a digital solution, leading to the birth of PACS in the 1980s. This marked a pivotal transition to digital, freeing Radiology departments from the constraints of physical film. The “Basics of Imaging Informatics: Part 1” article describes how PACS replaced film alternators with computer monitors, fundamentally changing the radiologist’s workstation.
The late 1990s and 2000s saw the widespread adoption of DICOM standards and the emergence of structured reporting systems. More recently, the landscape has been transformed by cloud computing and the rise of Artificial Intelligence (AI), particularly since 2012. As “Imaging Informatics: 25 Years of Progress” notes, the field has moved from managing static images to dynamic, intelligent systems.
The Transformative Role of Artificial Intelligence (AI)
Artificial Intelligence (AI) is no longer a futuristic concept in Radiology; it’s a present-day reality rapidly reshaping the practice. The integration of AI tools represents one of the most significant advancements in informatics in Radiology, promising to improve efficiency, accuracy, and patient outcomes.
What is AI in Radiology?
AI in Radiology involves computer programs performing tasks that traditionally require human intelligence. This includes Machine Learning (ML), where algorithms learn from data, and Deep Learning (DL), a subset of ML using complex neural networks that excel at image recognition.
These technologies are applied in various ways:
- Computer-Aided Detection (CADe): Systems that highlight potential abnormalities, drawing the radiologist’s attention to areas of interest. The first successful CAD system was implemented in 1994 for mammography.
- Computer-Aided Diagnosis (CADx): More advanced systems that assess the probability of disease or characterize a finding.
- Triage and Prioritization: AI algorithms can analyze incoming studies and flag critical cases (like suspected stroke) for immediate review.
- Quantitative Imaging: AI can precisely measure features in images, such as tumor volume changes, that are difficult for the human eye to assess.
As we dig deeper into “Developing, purchasing, implementing and monitoring AI tools in Radiology,” we see AI as a sophisticated assistant, enhancing the radiologist’s capabilities rather than replacing them.
Current AI Applications and Future Potential
The impact of AI on Radiology is already profound, with even more exciting potential on the horizon.
Current Applications:
- AI-assisted CT reading: Studies show AI can reduce reading time for radiologists by more than 44% when detecting findings like lung nodules and pleural effusions.
- Stroke and PE Detection: FDA-cleared AI algorithms help expedite the diagnosis of time-sensitive conditions like large vessel occlusions in stroke or pulmonary embolisms (PE).
- Workflow Optimization: AI can automate repetitive tasks like image sorting, measurements, and even drafting preliminary reports.
- Predictive Analytics: AI can analyze imaging and clinical data to predict disease progression or treatment response.
Future Potential:
The future of AI in informatics in Radiology points towards increasingly personalized and precise medicine:
- Personalized Medicine: AI will help provide patient-specific recommendations by integrating vast arrays of data, from imaging to genomics.
- Radiogenomics: This emerging field uses AI to link imaging features with genomic patterns, offering deeper insights into disease.
- Multimodal AI: Combining imaging data with other clinical information (pathology reports, clinical notes) will open up new diagnostic possibilities.
- Patient Understanding: Large Language Models (LLMs) can help by translating complex Radiology reports into easy-to-understand language.
While AI presents immense opportunities, it’s a tool to complement human perception, not replace it. The goal is to augment radiologists’ capabilities, making them “faster, better, cheaper,” as suggested in “Medical Imaging Informatics: How It Improves Radiology Practice Today.”
Benefits and Challenges in Modern Radiology
The adoption of robust informatics in Radiology systems brings a wealth of benefits, but this technological revolution also introduces challenges that must be addressed.
The Benefits: A Brighter Future for Radiology
- Improved Workflow: Informatics systems streamline the entire process from exam ordering to report distribution, allowing more time for patient care. As noted in “Medical Imaging Informatics: How It Improves Radiology Practice Today,” even small time savings, like 12 seconds per case, significantly boost efficiency.
- Improved Diagnostic Accuracy: With AI assistance, structured reporting, and instant access to prior exams, radiologists have more comprehensive information, leading to more accurate and timely diagnoses.
- Increased Efficiency: Automation, faster image retrieval, and streamlined communication reduce turnaround times, which is critical in emergency settings.
- Remote Reading (Teleradiology): Informatics enables radiologists to interpret studies from anywhere, ensuring continuous coverage for facilities like rural hospitals.
- Better Patient Outcomes: Timely, accurate diagnoses lead to earlier treatment. Reduced unnecessary repeat exams lower costs and minimize patient radiation exposure. For example, EHR interventions can increase lung cancer screening by 30%, directly impacting preventative care.
Overcoming Implementation Problems and Limitations
Despite the advantages, integrating advanced informatics in Radiology systems presents several problems.
- Data Security (HIPAA): Protecting sensitive patient information is paramount. With vast amounts of data being transmitted digitally, robust cybersecurity measures and strict adherence to HIPAA are non-negotiable, as recent major cyberattacks have highlighted.
- Interoperability Issues: While standards like DICOM and HL7 help, proprietary elements can still hinder data exchange between different vendors’ systems, creating information silos and inefficiencies.
- High Implementation Costs: The initial investment in PACS, RIS, AI, and related infrastructure can be substantial. Thorough cost-benefit analyses are crucial before integrating new systems, as noted in “Implementing AI in Clinical Radiology.”
- Radiologist Burnout: While AI can alleviate burnout, poorly implemented systems can have the opposite effect. Errors in project planning, especially with tools like voice recognition (VR), can make radiologists up to 25% less efficient, causing frustration.
- AI “Hallucinations” and Bias: AI models can sometimes generate factually incorrect responses (“hallucinations”). Furthermore, AI trained on biased data can perpetuate healthcare disparities, requiring careful validation.
- Data Storage Management: The volume of digital images grows exponentially. Managing petabytes of data, ensuring timely retrieval, and planning for future storage needs are ongoing challenges.
Careers and Education in Imaging Informatics
The rapid evolution of informatics in Radiology has created a growing demand for skilled professionals who can bridge the gap between clinical Radiology and information technology.
Career Paths in Imaging Informatics
An Imaging Informatics Professional (IIP) is a diverse role, often described as handling “everything about Radiology that isn’t medical science.” These professionals are essential for curating datasets, developing software, and implementing AI applications. Career paths include:
- PACS Administrator: The frontline manager of the PACS, ensuring its smooth operation, troubleshooting issues, and training users.
- Clinical Applications Specialist: An expert on the technical and clinical aspects of imaging systems, responsible for training staff and optimizing workflows.
- Imaging Informatics Radiologist: A radiologist with specialized informatics training who plays a visionary and managerial role in system design and oversight. Research shows that hospitals with an involved MII radiologist often see higher efficiency.
- Medical Physicists, IT Professionals, and Developers: Roles that contribute expertise in image quality, network infrastructure, and data management.
Education and Certification
To thrive in this field, professionals need a solid foundation in both Radiology principles and informatics.
- Formal Education: Many professionals enter the field with backgrounds in radiologic technology, computer science, or biomedical engineering.
- Fellowship Training: For radiologists, sub-specialty training in imaging informatics is available after Board Certification in Diagnostic Radiology.
- Certification: The American Board of Imaging Informatics (ABII) offers the Certified Imaging Informatics Professional (CIIP) certification, which demonstrates foundational knowledge. Other certifications from organizations like PARCA and the American Board of Preventive Medicine (ABPM) also exist.
Here’s a list of key skills for an imaging informaticist:
- Technical Proficiency: Deep understanding of PACS, RIS, and EMR systems.
- Networking and Cybersecurity: Knowledge of network architecture and security best practices (e.g., HIPAA compliance).
- Data Management: Expertise in data storage, retrieval, and archiving.
- Interoperability Standards: Proficiency with DICOM, HL7, and IHE.
- Problem-Solving: Ability to troubleshoot complex technical and workflow issues.
- Clinical Workflow Knowledge: Understanding of Radiology operations.
- Communication Skills: Bridging the gap between technical and clinical teams.
- Project Management: Overseeing implementation projects.
- AI/Machine Learning Concepts: Familiarity with AI applications.
- Continuous Learning: A commitment to staying updated in a rapidly evolving field.
Professional organizations like the Society for Imaging Informatics in Medicine (SIIM) offer valuable resources for those interested in this career path, which is one of the best fields in medicine for lifelong learners.
The Future of Informatics in Radiology
The trajectory of informatics in Radiology is one of continuous innovation.
- Emerging Technologies: Advancements like photon-counting CT, handheld ultrasound devices, and wearable technology are bringing imaging closer to the point of care.
- Enterprise Imaging (EI): The trend towards consolidating all imaging data across an organization into a single, accessible system will accelerate, improving coordination and reducing data silos.
- Cloud-Native PACS: The shift to cloud-native solutions will become more prevalent, offering scalability, accessibility, and improved data security for flexible access and AI applications.
- Federated Learning for AI: This approach allows AI models to learn from decentralized data without the data leaving its source, ensuring privacy while improving AI robustness.
- The Role of the “MII Radiologist”: The Imaging Informatics Radiologist will be even more crucial in guiding the adoption of new technologies and ensuring AI tools are integrated effectively and ethically.
- Impact on Patient Care: These advancements will profoundly impact patient care through improved diagnostics and personalized treatment plans. For instance, EHR interventions can increase lung cancer screening by 30%, demonstrating how informatics can drive preventative care.
Conclusion
As we’ve explored, informatics in Radiology is the intricate web of systems, standards, and intelligence that underpins modern Radiology. From foundational PACS and RIS systems to the cutting-edge applications of Artificial Intelligence, informatics is continuously reshaping patient care.
We’ve seen how standards like DICOM and HL7 enable interoperability and traced the field’s evolution from Röntgen’s findy to the current era of AI-driven diagnostics. The benefits are clear: improved workflow, greater diagnostic accuracy, and better patient outcomes. However, significant challenges remain, including data security, high implementation costs, and the ethical considerations of AI.
The future of informatics in Radiology is bright, promising even greater efficiencies and precision. For professionals in Radiology, understanding and adapting to this evolving landscape is essential. The demand for skilled Imaging Informatics Professionals who can steer this complex terrain will only continue to grow.
At Scrubs CE, we believe in empowering healthcare professionals with the knowledge needed to excel in this dynamic environment. Continuous learning is the key to staying ahead and providing the highest quality of care.
Explore continuing education courses for radiologic technologists

Recent Comments