A New Window into the Human Body
Advanced imaging techniques are sophisticated medical technologies that create detailed pictures of the inside of your body to help doctors diagnose and treat diseases. Here are the main types:
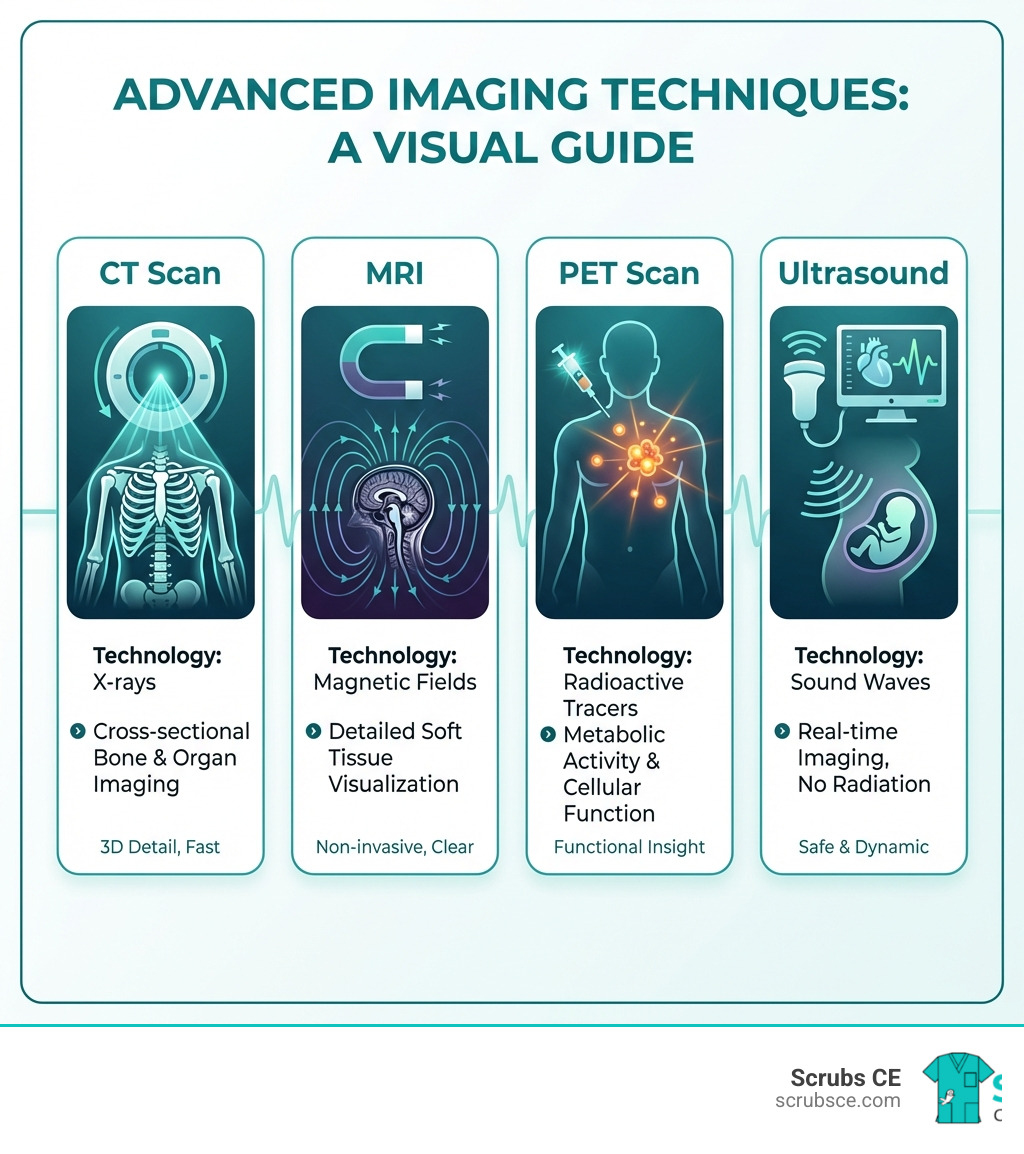
- CT (Computed Tomography) – Uses X-rays to create 3D cross-sectional images, best for bones, lungs, and detecting trauma
- MRI (Magnetic Resonance Imaging) – Uses magnetic fields and radio waves to visualize soft tissues like the brain, muscles, and organs
- PET (Positron Emission Tomography) – Tracks metabolic activity using radioactive tracers to detect cancer and brain disorders
- Ultrasound – Uses sound waves to create real-time images, commonly used in pregnancy and cardiac imaging
- Fluoroscopy – Provides continuous X-ray imaging for real-time guidance during procedures
When Wilhelm Conrad Röntgen finded X-rays in 1895, he gave medicine its first glimpse inside the living human body without surgery. That breakthrough launched over a century of innovation.
Modern advanced imaging techniques now go far beyond simple X-rays. They can show not just what your organs look like, but how they function. Some techniques reveal anatomical structure in stunning detail. Others track metabolic processes at the cellular level.
The numbers tell the story of imaging’s explosive growth. Worldwide, approximately 5 billion medical imaging studies had been conducted by 2010. In the United States alone, CT scans jumped from 72 million in 2007 to 80 million in 2015. Today, medical imaging accounts for about 50% of total ionizing radiation exposure in the U.S.
This growth reflects imaging’s central role in modern healthcare. Advanced techniques help doctors detect diseases earlier, guide treatments more precisely, and monitor patient progress more effectively. They are essential for diagnosing everything from broken bones to brain tumors to heart disease.
The field keeps evolving rapidly. Hybrid systems like PET/CT combine anatomical and functional imaging in a single scan. Artificial intelligence now helps radiologists analyze images faster and more accurately. New techniques promise better image quality with less radiation exposure.
For imaging professionals, staying current with these advances is both a challenge and an opportunity. Understanding how different modalities work, when to use them, and how to minimize risks helps you provide better patient care and advance your career.
I’m Zita Ewert, and I’ve spent my career helping Radiology technologists and imaging professionals steer the rapidly evolving landscape of medical imaging through accessible continuing education at SCRUBS CE. Understanding advanced imaging techniques is essential for maintaining certification and delivering safe, high-quality patient care in today’s diagnostic environment.
Explore more about advanced imaging techniques:
The Core Modalities: A Deep Dive into CT, MRI, and PET Scans
At the heart of modern medical diagnostics are three foundational advanced imaging techniques: Computed Tomography (CT), Magnetic Resonance Imaging (MRI), and Positron Emission Tomography (PET). Each offers a unique window into the human body, providing key information for diagnosis, treatment planning, and monitoring. Let’s explore these modalities.
Computed Tomography (CT)
Fundamental principles: Imagine taking hundreds of X-ray pictures from every angle around your body. That’s essentially what a CT scan does! It uses rotating X-ray beams and highly sensitive detectors to capture a series of cross-sectional (slice-like) images. These individual slices are then processed by a computer to create detailed two-dimensional images and even sophisticated 3D models of organs, bones, and soft tissues. The principle relies on the varying absorption of X-rays by different tissue densities—denser tissues like bone absorb more X-rays and appear white, while less dense tissues appear darker.
Clinical applications: CT scans are workhorses in Radiology. Their speed and detail make them indispensable for diagnosing trauma, such as internal injuries or fractures, often in emergency situations. We use them extensively for cancer staging, helping to locate tumors and assess their spread. They are also crucial for evaluating vascular diseases, identifying blockages or aneurysms, and providing intricate detail of bone structures, which is vital for orthopedic planning. Indeed, CT scan is considered the best method for detecting and recording modifications in tumor mass during treatment.
Benefits: A major advantage of CT is its speed, allowing for rapid diagnosis, especially in critical care. It provides excellent spatial resolution for bone and lung tissues, and the ability to reconstruct detailed 3D representations is a game-changer for surgical planning.
Limitations and Risks: The primary limitation and risk associated with CT scans is their use of ionizing radiation. This exposure, while low per scan, accumulates and carries a slight, increased cancer risk. In the United States, medical imaging, including CT, accounts for approximately 50% of the total ionizing radiation exposure. The sheer volume of scans performed highlights this concern: almost 72 million CT scans were conducted in the U.S. in 2007, rising to 80 million in 2015. Therefore, we emphasize the importance of adhering to the ALARA (As Low As Reasonably Achievable) principle to minimize radiation dose without compromising diagnostic quality. For more information on radiation exposure, you can review scientific research on CT radiation exposure.
Consider enhancing your expertise in this critical area with Computed Tomography (CT) Courses or Cardiac and Vascular Computed Tomography. If you’re looking for CT CEU Credits, we have resources for you too!
Magnetic Resonance Imaging (MRI)
Fundamental principles: MRI takes a completely different approach, using powerful magnetic fields and radio waves instead of X-rays. Our bodies are mostly water, and water molecules contain hydrogen atoms. When placed in a strong magnetic field, the protons within these hydrogen atoms align with the field. Short bursts of radio waves temporarily knock these aligned protons out of alignment. When the radio waves are turned off, the protons relax back into alignment, releasing energy signals. These signals are detected by the MRI scanner and converted into highly detailed images. Because it primarily images hydrogen, which is abundant in water, MRI excels at visualizing soft tissues.
Clinical applications: MRI is our go-to for unparalleled soft tissue analysis. It’s invaluable for diagnosing neurological disorders such as multiple sclerosis, brain tumors, stroke, and spinal cord injuries. We also rely on it heavily for musculoskeletal injuries, clearly showing ligaments, tendons, cartilage, and muscles that might be missed by other methods. As one statistic highlights, MRI has revealed lesions in 27-37% of patients that were not detected by mammography, underscoring its superior soft tissue sensitivity.
Benefits: The key benefit of MRI is its exceptional soft tissue contrast, allowing clear differentiation between various tissues. Crucially, it does not use ionizing radiation, making it a safer option for repeated scans or for sensitive populations like pregnant women (though MRI without contrast is generally preferred during pregnancy).
Risks: While generally safe, MRI does have considerations. Some patients experience claustrophobia due to the enclosed space of the scanner. More importantly, strong magnetic fields mean that individuals with certain metal implants (like pacemakers, some surgical clips, or metallic foreign bodies) cannot undergo an MRI due to safety risks.
Interested in mastering MRI? Explore our Magnetic Resonance Imaging (MRI) Courses and dig into MRI Training Requirements or find What is Involved in MRI Training?. We also offer critical information on MRI Safety: Things You Should Know.
Positron Emission Tomography (PET)
Fundamental principles: PET scans offer a unique functional view of the body, focusing on metabolic activity rather than just anatomy. We introduce a small amount of a radioactive substance, called a radiotracer, into the patient’s bloodstream. This radiotracer is usually tagged to a molecule like glucose (FDG), which is naturally taken up by cells. As the radiotracer decays, it emits positrons. When a positron collides with an electron in the body, they annihilate each other, producing two gamma rays that travel in opposite directions. The PET scanner detects these gamma rays, and a computer reconstructs a 3D image showing areas of high metabolic activity, indicating cellular function.
Clinical applications: PET scans are particularly powerful in oncology, as cancer cells often have higher metabolic rates than healthy cells, making them “light up” on a PET scan. This helps us detect cancer, determine its stage, and monitor treatment effectiveness. In neurology, PET is invaluable for diagnosing conditions like Alzheimer’s and Parkinson’s diseases, by revealing changes in brain activity. For instance, an early diagnosis of Alzheimer’s disease can be scanned by PET technology with an impressive 93% accuracy. We also use PET in cardiology to assess blood flow and heart function.
Benefits: The primary benefit of PET is its ability to detect diseases at a cellular or molecular level, often before structural changes are visible on CT or MRI. This enables early disease detection and can significantly impact treatment outcomes.
Risks: Like CT, PET involves exposure to ionizing radiation from the radiotracer. While the dose is carefully controlled, it’s a factor we always consider.
Limitations: PET scans typically have lower spatial resolution compared to CT or MRI, meaning they don’t provide as sharp anatomical detail. This is why hybrid systems, which we’ll discuss later, are so valuable.
Deepen your understanding of this cutting-edge modality with our Nuclear Medicine and PET CT courses.
| Modality | Principle | Best For | Risks | Cost (Relative) |
|---|---|---|---|---|
| CT | X-ray absorption, cross-sectional images | Bone, trauma, lungs, internal bleeding, cancer staging | Ionizing radiation, contrast reactions | Moderate |
| MRI | Magnetic fields, radio waves, hydrogen atoms | Soft tissue, brain, spinal cord, joints, ligaments | Strong magnetic fields (metal implants), claustrophobia | High |
| PET | Radiotracers, metabolic activity | Cancer detection/staging, brain function, heart viability | Ionizing radiation (radiotracer) | High |
| Ultrasound | Sound waves, real-time echoes | Soft tissues, blood flow, pregnancy, guidance for procedures | Generally none (non-ionizing) | Low |
A Spectrum of Advanced Imaging Techniques
Beyond the big three, a diverse array of advanced imaging techniques continues to expand our diagnostic toolkit. These modalities offer unique advantages, from real-time visualization to highly specialized surface analysis, further enhancing our ability to understand and treat complex medical conditions.
The Evolution of Ultrasound Imaging
How ultrasound works: Ultrasound imaging uses high-frequency sound waves, far beyond the range of human hearing. A transducer emits these sound waves into the body. When the waves encounter different tissues or structures, they bounce back as echoes. The transducer then detects these echoes, and a computer processes them to create real-time images. It’s like sonar for your body!
Evolution from 2D to 3D/4D: What started as simple 2D black-and-white images has evolved dramatically. Modern systems offer 3D ultrasound, providing volumetric views, and even 4D ultrasound, which adds the dimension of time, allowing us to see movement in real-time—a truly magical experience when observing a fetus. Doppler ultrasound is another advancement, using changes in sound wave frequency to visualize and measure blood flow, critical for assessing cardiovascular health.
Current applications: Ultrasound is incredibly versatile. In obstetrics, it’s essential for monitoring fetal development, assessing growth, and detecting potential abnormalities. In cardiology, echocardiography uses ultrasound to visualize the heart’s structure and function, including blood flow through its chambers and valves. It’s also widely used for abdominal imaging (liver, kidneys, gallbladder), musculoskeletal imaging (tendons, muscles, ligaments), and guiding biopsies or other interventional procedures.
Advantages: Ultrasound’s popularity stems from several key advantages. It’s highly portable, meaning we can bring the scanner to the patient’s bedside. It provides real-time imaging, allowing dynamic assessment of organs and blood flow. Most importantly, it uses no ionizing radiation, making it incredibly safe, particularly for pregnant patients. Furthermore, ultrasound is comparatively less expensive than other imaging techniques like MRI and CT, making it widely accessible.
Fluoroscopy: Imaging in Real-Time
What is fluoroscopy: If you’ve ever watched a live X-ray “movie” of someone swallowing barium, you’ve seen fluoroscopy in action. It’s an advanced imaging technique that uses a continuous X-ray beam to create real-time, moving images of the inside of the body. Think of it as a live video feed, allowing us to observe the dynamic processes of internal organs.
How it’s used: Fluoroscopy is invaluable for guiding various medical procedures. In interventional Radiology, it helps us precisely place catheters, stents, or other devices within blood vessels or organs. Barium studies use fluoroscopy to visualize the gastrointestinal tract, helping to diagnose conditions like ulcers, strictures, or reflux. It’s also used in orthopedic surgery to guide joint injections or verify proper placement of hardware during procedures.
Benefits: The primary benefit of fluoroscopy is its ability to provide real-time guidance. This allows physicians to make immediate adjustments during complex procedures, significantly improving precision and safety.
Risks: Because it uses a continuous X-ray beam, fluoroscopy can involve a higher radiation dose compared to a single static X-ray image. We employ strict protocols and the ALARA principle to minimize patient and staff exposure during these procedures.
For those interested in the intricacies of real-time imaging, our Vascular and Interventional Radiology course offers comprehensive insights.
Specialized 2D Advanced Imaging Techniques
While many advanced imaging techniques focus on creating volumetric (3D) images of internal structures, some specialized 2D techniques offer incredible detail about surfaces and material properties. These are particularly prominent in fields like cultural heritage preservation and material science, but their principles can inform medical applications.
- Polynomial Texture Mapping (PTM) / Reflectance Change Imaging (RTI): These techniques involve taking multiple images of an object under different lighting conditions. By capturing how light reflects off a surface from various angles, we can then computationally re-light the object during viewing. This allows us to manipulate the light to highlight incredibly subtle surface details, such as fine incisions on ancient artifacts like the Antikythera Mechanism, which might be invisible under normal light.
- Multispectral Imaging / Hyperspectral Imaging: These methods go beyond the visible light spectrum (red, green, blue) to capture a material’s spectral reflectance across a much wider and finer range of the electromagnetic spectrum. This rich data allows us to accurately reproduce colors, distinguish between different materials (like various inks in a manuscript), and even classify substances based on their unique spectral signatures.
- X-ray Fluorescence (XRF): This technique involves bombarding a surface with X-rays, which causes the atoms in the material to emit characteristic secondary X-rays (fluorescence). By analyzing these fluorescent X-rays, we can identify and quantify the elemental composition of the surface. Researchers at Cornell, for example, have used XRF to reveal trace elements left by painting or chisel work on ancient stone inscriptions, providing insights into their history.
Difference from volumetric techniques: The key distinction here is that these specialized 2D techniques focus on detailed surface characteristics and material composition rather than penetrating the object to reveal its internal 3D structure. While a CT scan shows us the inside of a bone, PTM might show us the texture of its outer surface, and multispectral imaging could tell us about the pigments used on an archaeological artifact. In medicine, these principles can be adapted for highly detailed surface analysis in dermatology or ophthalmology, or for analyzing tissue samples.
The Power of Fusion and the Future of Radiology
The relentless pursuit of clearer, more comprehensive diagnostic information continues to drive innovation in medical imaging. Two exciting frontiers are the development of hybrid imaging systems that combine the strengths of different modalities, and the emergence of new technologies, including the transformative power of Artificial Intelligence.
Hybrid Imaging: The Best of Both Worlds
What is hybrid imaging: Why choose when you can have both? Hybrid imaging combines two different advanced imaging techniques into a single scanner, allowing us to acquire anatomical and functional information simultaneously. The most common examples are PET/CT and PET/MRI.
- PET/CT: This combines the metabolic insights of a PET scan with the detailed anatomical images of a CT scan. The CT component provides precise localization of the metabolic “hot spots” detected by the PET, offering a comprehensive view. This is particularly powerful in oncology, where it allows us to accurately stage cancer, assess treatment response, and differentiate between active tumor tissue and scar tissue.
- PET/MRI: This even newer hybrid combines PET’s functional data with MRI’s superior soft tissue contrast and lack of ionizing radiation. PET/MRI is gaining traction in neurology, pediatric imaging, and for certain cancers, providing highly detailed anatomical context for metabolic changes without additional radiation dose.
Fusing anatomical and functional data: The magic of hybrid imaging lies in this fusion. It provides a more complete picture of disease processes. Instead of looking at two separate images and trying to mentally overlay them, we get a single, co-registered dataset. This leads to improved diagnostic capabilities, especially in complex cases, and significantly improved accuracy in cancer staging and treatment planning. The synergistic benefits mean that the combined information is often greater than the sum of its parts, leading to more confident diagnoses and better patient management.
Emerging Advanced Imaging Techniques on the Horizon
The future of Radiology is brimming with possibilities, promising even more precise, safer, and personalized diagnostic tools.
Future outlook: We are seeing rapid advancements driven by several key areas.
- Artificial Intelligence (AI) in Radiology: AI and machine learning are revolutionizing how we process, analyze, and interpret medical images. AI algorithms can rapidly sift through vast amounts of data, identify subtle patterns, and even highlight potential abnormalities that might be missed by the human eye. This leads to faster image analysis, aids diagnostic accuracy by providing quantitative measurements, and can even offer predictive analytics regarding disease progression. AI aims to reduce the workload on radiologists, allowing them to focus on the most complex cases and patient interaction. You can learn more about how AI is changing the field in 5 Trends Transforming Radiology Continuing Education You Need to Know.
- Quantitative Imaging: Moving beyond subjective visual assessment, quantitative imaging extracts measurable biomarkers from medical images. This allows for objective, repeatable metrics to track disease progression or response to therapy, paving the way for truly personalized medicine.
- Molecular Imaging: This field aims to visualize biological processes at the molecular and cellular level in vivo. It involves developing highly specific probes that target particular molecules or pathways involved in disease, offering extremely early detection and precise characterization.
- New X-ray Sources: Innovations like Carbon Nanotube X-Ray Sources are ready to significantly improve image quality while drastically reducing radiation dose. This technology, highlighted in latest research on Carbon Nanotube X-Ray Sources, promises more efficient X-ray generation and a leap forward in the safety and efficacy of X-ray-based imaging. This kind of research is crucial for advancing advanced imaging techniques.
- 4D Imaging: We’re already seeing the rise of 4D CT, 4D ultrasound, and 4D MRI, which add the dimension of time to 3D imaging. This allows for dynamic assessment of moving organs (like the heart or lungs) and provides invaluable insights into physiological processes.
These emerging advanced imaging techniques are not just incremental improvements; they represent a paradigm shift in how we approach diagnosis and treatment, promising a future of even greater precision and patient safety.
Frequently Asked Questions about Advanced Imaging
We often get questions about the different advanced imaging techniques available today. Here are some of the most common ones we hear, along with our expert answers.
What is the most detailed imaging technique?
The “most detailed” imaging technique really depends on what we’re trying to look at!
- For unparalleled detail of soft tissues, such as the brain, spinal cord, muscles, ligaments, and most internal organs, MRI typically provides the highest resolution and best contrast. It’s like having a microscopic view without the surgery.
- When we need to see bone structures, complex fractures, or detailed views of the lungs, CT scans are usually superior due to their excellent spatial resolution for dense tissues.
- If we’re interested in metabolic function or cellular activity, for example, to detect cancer spread or assess brain activity in neurological disorders, PET scans are the most detailed in terms of functional information, even if their anatomical resolution isn’t as high as MRI or CT.
- For real-time visualization and dynamic processes, especially in obstetrics or cardiology, ultrasound offers excellent detail without radiation.
So, it’s not a one-size-fits-all answer, but rather about choosing the right tool for the job.
Which advanced imaging techniques use radiation?
Understanding radiation exposure is crucial for patient safety. Here’s a breakdown:
-
Ionizing Radiation Sources:
- CT scans (Computed Tomography) use X-rays.
- PET scans (Positron Emission Tomography) use radioactive tracers that emit positrons, leading to gamma ray emission.
- Fluoroscopy uses continuous X-ray beams for real-time imaging.
- Standard X-rays (Projectional Radiography) also use ionizing radiation.
We carefully manage the doses from these modalities to ensure patient safety, always adhering to the ALARA principle.
-
Non-Radiation Techniques:
- MRI (Magnetic Resonance Imaging) uses strong magnetic fields and radio waves, not ionizing radiation.
- Ultrasound uses high-frequency sound waves, making it a very safe option, especially for pregnant women and children.
We always weigh the diagnostic benefits against the potential risks of radiation exposure, choosing the safest and most effective imaging modality for each patient’s specific needs.
How is AI changing medical imaging?
Artificial Intelligence (AI) is rapidly changing medical imaging in profound ways, making Radiology more efficient and precise:
- Faster Image Analysis: AI algorithms can process vast numbers of images much quicker than humans, flagging abnormalities and helping radiologists prioritize cases.
- Aiding Diagnostic Accuracy: AI can detect subtle changes or patterns that might be missed, improving the accuracy of diagnoses, especially in complex conditions like early-stage cancers or neurological changes. It helps in quantitative analysis, providing objective measurements that support clinical decisions.
- Predictive Analytics: Beyond diagnosis, AI can analyze imaging data to predict disease progression, treatment response, or even the risk of future events, moving us towards proactive healthcare.
- Reducing Radiology Workload: By automating routine tasks and pre-screening images, AI can significantly reduce the cognitive load and burnout experienced by radiologists, allowing them to focus their expertise where it’s most needed.
AI is not replacing radiologists, but rather empowering them with advanced tools to improve their capabilities and improve patient care. It’s an exciting frontier in the evolution of advanced imaging techniques.
Conclusion: The Ever-Expanding Frontier of Medical Vision
We’ve journeyed through the intricate world of advanced imaging techniques, from the foundational principles of CT, MRI, and PET scans to the dynamic insights of ultrasound and fluoroscopy, and the specialized detail of 2D surface imaging. We’ve seen how hybrid systems combine strengths and how emerging technologies like AI are ready to redefine the future of Radiology.
The critical role of imaging in early disease detection and treatment planning cannot be overstated. These technologies allow us to peer inside the human body with unprecedented clarity, catching diseases earlier, guiding interventions with greater precision, and monitoring patient progress more effectively. This shift towards personalized medicine means treatments can be custom based on a patient’s unique biological information, gleaned from these sophisticated images.
The future trends in advanced imaging techniques point towards even greater integration, intelligence, and safety. AI will continue to improve diagnostic capabilities, new physics will open up even higher resolution and lower radiation doses, and molecular imaging will push the boundaries of early detection.
For us, as healthcare professionals, staying abreast of these rapid developments is not just about professional growth; it’s about providing the best possible care for our patients. Our commitment to continuing education at ScrubsCE.com ensures that you have access to the latest knowledge and skills needed to excel in this ever-expanding frontier of medical vision.
Ready to advance your knowledge and career in Radiology? Find More info about our Radiology CE courses and stay at the forefront of medical imaging innovation.

Recent Comments