Why Bariatric CT Imaging Matters in Today’s Healthcare Landscape
Bariatric CT imaging refers to the specialized computed tomography protocols and techniques used to image obese patients, who present unique challenges including equipment limitations, increased image noise, and radiation dose considerations. With approximately 42% of US adults now classified as obese and up to 21% of healthcare expenditures directed toward obesity-related diseases, understanding how to effectively image this growing patient population has become essential for radiologic technologists.
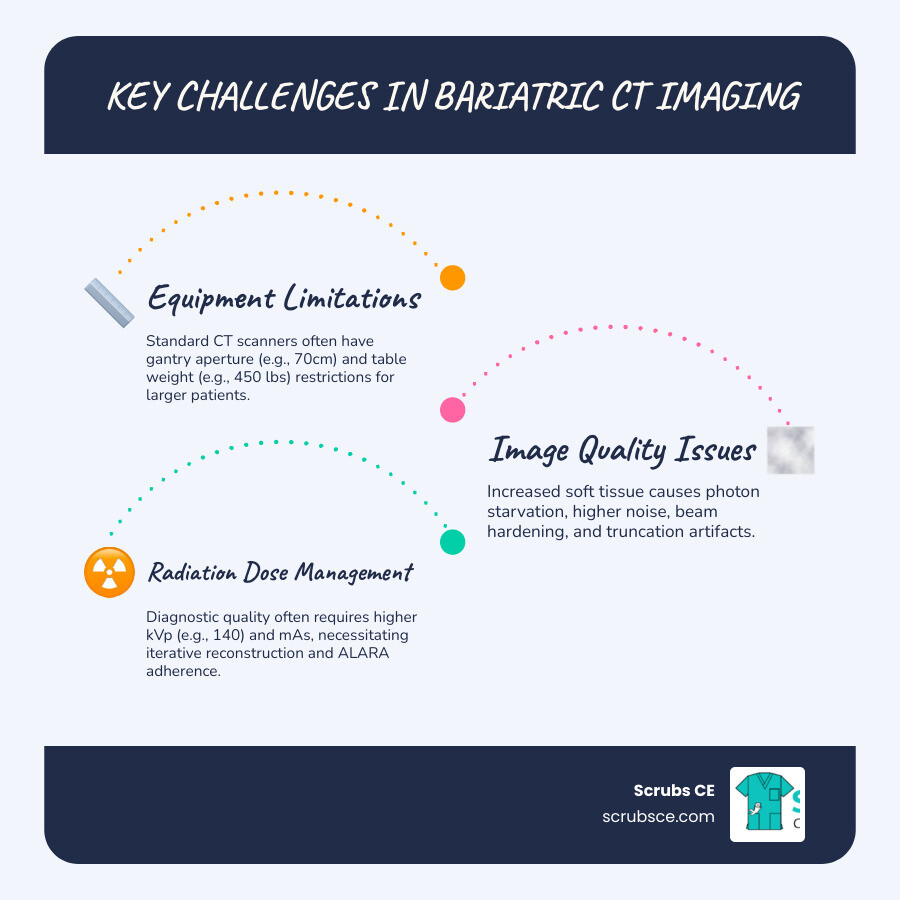
Key Challenges in Bariatric CT Imaging:
- Equipment Limitations – Standard CT scanners may not accommodate patients exceeding weight limits (typically 450 lbs) or girth restrictions (70 cm gantry aperture minus 15-18 cm table width)
- Image Quality Issues – Increased soft tissue depth leads to photon starvation, higher noise levels, and artifacts like beam hardening and truncation
- Radiation Dose Management – Obese patients often require higher radiation doses to achieve diagnostic image quality, raising ALARA concerns
- Contrast Protocol Adjustments – Altered hemodynamics in obesity require modified injection rates, timing, and total iodine mass calculations
The rise in bariatric surgery—with complication rates of only 4% and mortality of just 0.1%—has further increased the need for quality pre- and post-operative imaging. Yet many technologists receive limited training on adapting standard protocols for this patient population.
As Zita Ewert, I’ve dedicated my career to ensuring imaging professionals have access to practical, regulatory-compliant continuing education on evolving topics like Bariatric CT imaging. Through SCRUBS Continuing Education, we’ve developed specialized courses that address real-world challenges technologists face daily when working with diverse patient populations.
This guide walks you through the technical considerations, protocol modifications, and interpretive pitfalls you need to know when performing CT scans on bariatric patients—from understanding equipment requirements to recognizing post-surgical complications.
The “Weighty” Challenges of Bariatric CT Imaging
Imaging our bariatric patients comes with a unique set of technical problems. The sheer size of these individuals often pushes the limits of standard imaging equipment, leading to a cascade of challenges from patient accommodation to image quality. The primary technical challenges begin before the scan even starts: will the patient fit, and can our equipment handle their weight?
Essential equipment requirements for effective Bariatric CT imaging include CT scanners with adequate table load limits, which historically stood around 450 lbs (204 kg) but now can reach up to 680 lbs (308 kg) in newer bariatric models. Equally crucial is a large gantry aperture, traditionally 70 cm in diameter, but now available up to 90 cm. When assessing patient girth, we must remember to subtract the table width (typically 15-18 cm) from the gantry aperture. This means a 90 cm gantry might only accommodate patients up to 72-75 cm in girth. A large scan field of view (FOV) is also vital to ensure comprehensive anatomical coverage without cropping, which can lead to critical diagnostic information being lost from subcutaneous tissues. Finally, high-power generators are necessary to deliver the increased X-ray tube output needed for larger patients.
Once the patient is accommodated, the next challenge is image quality. Increased soft tissue thickness leads to more X-ray attenuation, resulting in “photon starvation” at the detectors. This manifests as increased image noise, making it harder to distinguish fine details and potentially obscuring pathology. To compensate, higher radiation doses are often required, raising concerns about adhering to the ALARA (As Low As Reasonably Achievable) principle. Balancing diagnostic image quality with radiation dose management is a constant tightrope walk in Bariatric CT imaging. For more in-depth information on the technical aspects of radiography, we recommend exploring our courses on Radiologic Science for Technologists. You can also learn more about technical challenges in imaging obese patients in the emergency setting.
Mitigating Image Noise and Artifacts
Obesity isn’t just about size; it introduces specific artifacts that can severely compromise image interpretation. These obesity-related artifacts include beam hardening, where the X-ray beam becomes “harder” (more energetic) as it passes through dense tissue, leading to streaking artifacts. Truncation artifacts occur when a patient’s body extends beyond the scan field of view (SFOV), causing incomplete data acquisition. Cropping artifacts are a consequence of this truncation, where the reconstructed image literally “crops” out parts of the patient. Finally, ring artifacts can appear due to detector malfunction or calibration issues, but their impact can be magnified in larger patients due to higher X-ray attenuation.
To combat these challenges, we employ several mitigation strategies. Iterative reconstruction (IR) methods are game-changers, processing raw data multiple times to reduce noise and improve image quality while potentially lowering radiation dose. Increasing the tube voltage (kVp), often to 140 kV, helps the X-ray beam penetrate denser tissue more effectively. Simultaneously, an increased tube current (mAs) delivers more photons, improving signal-to-noise ratio. For emergency abdominal CT in obese patients using third-generation dual-source CT, studies show good image quality can be achieved, though radiation dose increases with higher BMI. Slower gantry rotation can also increase the effective mAs, further boosting signal. However, this must be balanced against the risk of motion artifacts. Understanding these nuances is crucial for accurate image analysis, and our Radiographic Image Analysis courses dig deeper into such interpretive skills.
Special Considerations for Contrast-Improved CT
When performing contrast-improved CT scans in obese patients, we face additional complexities. Obesity alters a patient’s hemodynamics, leading to increased cardiac output and a larger blood volume. This means the contrast material gets diluted more, and its transit time through the body can be different. To achieve optimal vascular improvement, we often need to adjust the injection rate, frequently increasing it to >5-6 ml/second for pulmonary embolism studies and 6-7 cc/second for cardiac CT in severe obesity.
Precise scan timing is also paramount. A delay or acceleration in contrast arrival can lead to suboptimal improvement of the target vessels or organs. Calculating the total iodine mass becomes more critical, as under-dosing can result in poor image quality, while over-dosing increases patient risk. Achieving optimal vascular improvement is often the primary goal, but parenchymal improvement can be challenging due to the increased tissue volume and contrast dilution. These physiological considerations require careful planning and execution to ensure diagnostic quality. For those looking to deepen their understanding of contrast dynamics and cardiovascular imaging, our Cardiac and Vascular Computed Tomography courses offer comprehensive insights.
Common Findings and Interpretive Pitfalls in Bariatric Patients
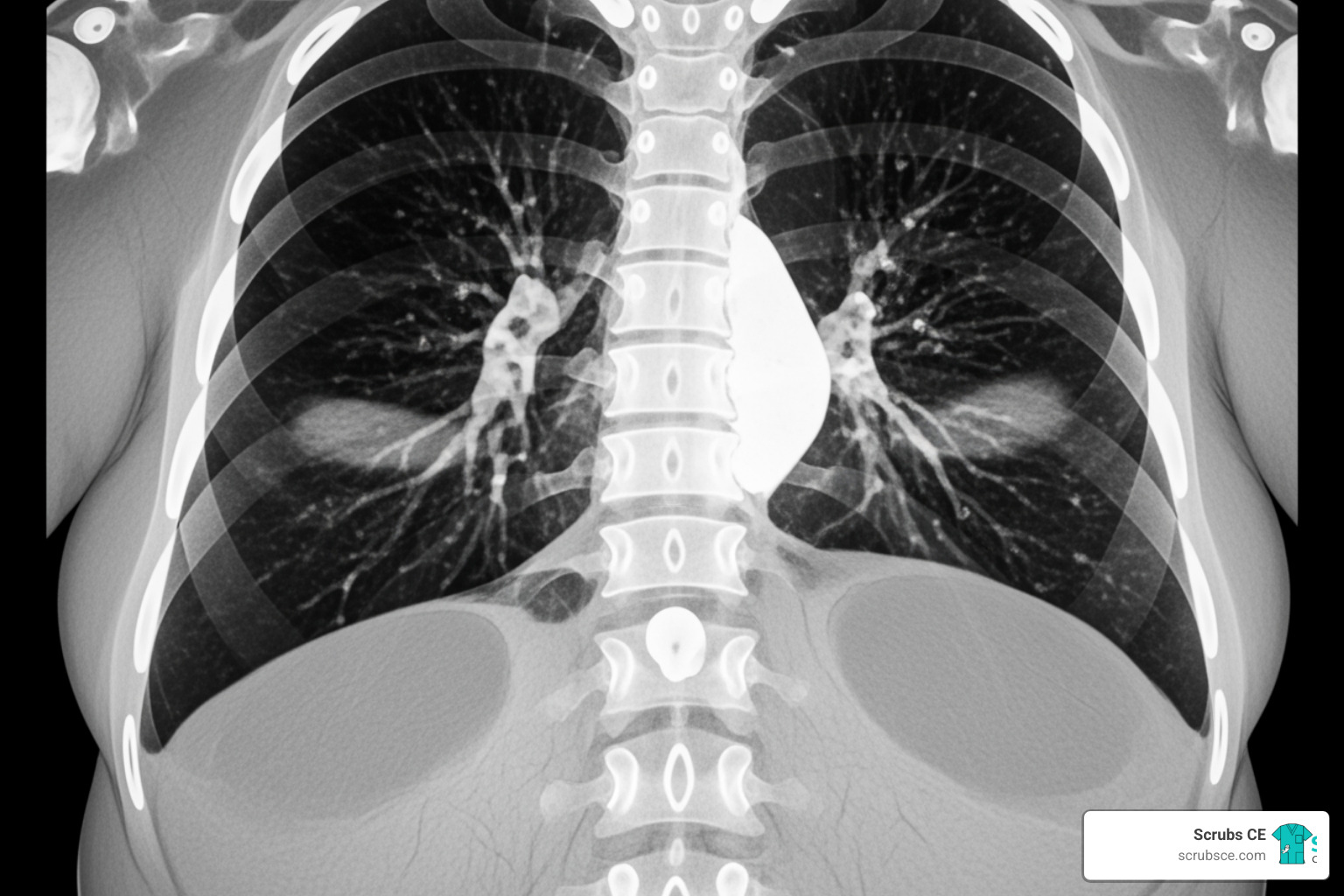
Interpreting CT scans of obese patients, especially chest CTs, requires a keen eye and an understanding of how excess weight impacts anatomy and physiology. The effects of obesity on the lungs are profound, driven by both mechanical and metabolic factors. Increased abdominal fat pushes the diaphragm upwards, leading to reduced lung volumes, particularly at the bases.
Typical chest CT findings in obese patients often include basilar atelectasis (collapsed lung tissue), which appears as wedge-shaped opacities in the lower lung lobes. We might also observe tracheal deviation, increased epicardial fat (fat surrounding the heart), and a higher risk of pulmonary embolism due to obesity-associated coagulation changes. The underlying pathological mechanisms involve decreased functional residual capacity, increased airway closure, and altered gas exchange.
However, interpreting these findings comes with potential pitfalls. A common one is misinterpreting skin folds as pneumothorax or other pathology. These folds, especially prominent in obese patients, can cast linear shadows that mimic lung collapse. The increased soft tissue can also obscure subtle findings, making detection of small nodules or early inflammatory changes more difficult. Awareness of these characteristic imaging features and potential traps is crucial for avoiding misdiagnosis. Our Body CT Secrets course offers valuable insights into interpreting complex body CT scans, including those of bariatric patients.
The Future of Bariatric CT Imaging: AI and Body Morphometry
The landscape of Bariatric CT imaging is rapidly evolving, with Artificial Intelligence (AI) and body morphometry emerging as powerful tools. AI in radiology is moving beyond simple image improvement, now contributing significantly to quantitative analysis. Body morphometry, the science of measuring and analyzing body shape and composition, is particularly relevant here.
AI-driven software can perform automated tissue segmentation, carefully differentiating between visceral fat (around organs) and subcutaneous fat (under the skin). This allows for precise quantification of fat distribution, which is a better indicator of metabolic health than BMI alone. It can also assess sarcopenia, the loss of muscle mass, which is surprisingly common in obese individuals and impacts surgical outcomes.
Beyond body composition, AI and body morphometry are being used for predictive analytics. For instance, these tools can aid in lung cancer risk prediction by analyzing lung nodule characteristics and body composition, providing a more personalized risk assessment. They are also being explored for COVID-19 outcome prediction, helping to identify obese patients at higher risk for severe disease. The ability to extract such nuanced insights from standard CT scans is revolutionizing our understanding of obesity-related health risks and tailoring patient care. These insights into AI and body morphometry highlight a future where imaging is not just diagnostic but also predictive.
The Role of Bariatric CT Imaging in Lung Cancer Screening
Lung cancer screening with low-dose CT (LDCT) has shown significant benefits in reducing mortality for high-risk individuals. However, applying LDCT to obese patients introduces its own set of challenges. The increased body habitus often means higher technical parameters are needed, potentially increasing the radiation dose and compromising the “low-dose” aspect of the screen.
Protocol optimization is key here. We must carefully adjust kVp and mAs settings, often using iterative reconstruction, to maintain diagnostic image quality while keeping the radiation dose as low as possible. Nodule detection accuracy can be affected by increased image noise and artifacts in obese patients, making subtle findings harder to identify. Therefore, the impact of body habitus on image quality is a constant consideration.
The goal is to ensure that obese patients, who often have a higher risk for various cancers, can still benefit from effective lung cancer screening without excessive radiation exposure. This requires a deep understanding of radiation physics and dose management. For comprehensive knowledge on keeping both patients and ourselves safe, our courses on Radiation Protection in Medical Radiography are invaluable.
Imaging After Bariatric Surgery: A Postoperative Guide
Bariatric surgery offers a new lease on life for many, but the journey doesn’t end in the operating room. Postoperative imaging plays a crucial role in monitoring patients, ensuring the surgical site is healing correctly, and swiftly detecting potential complications. The role of imaging is to provide early and precise identification of anastomotic integrity, patency, and any adverse events.
There’s an ongoing debate in the medical community regarding routine versus selective imaging after bariatric surgery. Some surgeons advocate for routine imaging immediately post-op (within the first two days) to catch asymptomatic leaks or other issues. Others prefer a selective approach, reserving imaging for symptomatic or high-risk patients. Our ACR Appropriateness Criteria provide evidence-based guidance to help steer these decisions.
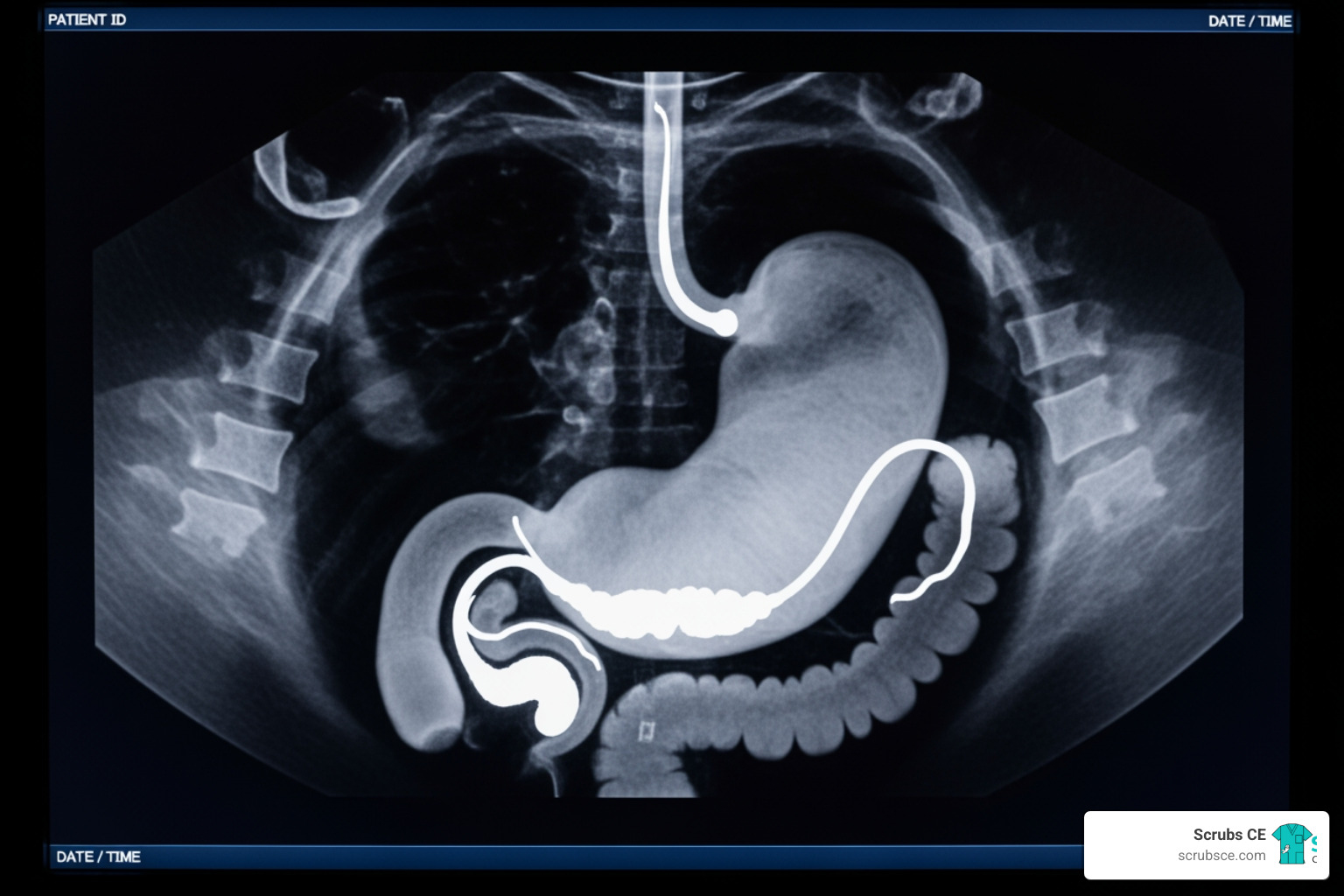
Common imaging modalities employed include fluoroscopic upper gastrointestinal (UGI) series, which are excellent for evaluating the integrity and patency of the new gastrointestinal anatomy, and CT scans, especially with intravenous contrast, for detecting a broader range of complications like abscesses or internal hernias. Ultrasound is often used for gallbladder evaluation, particularly given the increased risk of gallstones after rapid weight loss, and bone density scans (DEXA) monitor for potential changes in bone mineral density.
The effectiveness of these modalities can vary, particularly for critical complications like anastomotic leaks. While UGI series has a high specificity (100%), its sensitivity for detecting leaks within two days post-op is only around 54%. CT, on the other hand, boasts a pooled sensitivity of 91% and a mean specificity of 99.7% for leak detection. For detecting an anastomotic leak, the comparison is as follows:
- UGI Series: Sensitivity 54%, Specificity 100%
- CT with IV Contrast: Sensitivity 91-95%, Specificity 99.7-100%
This data illustrates why CT is often favored for suspected complications, offering a more comprehensive view.
Common Post-Surgical Complications and Their Imaging Signs
After bariatric surgery, we’re on the lookout for several potential complications, each with tell-tale imaging signs. Anastomotic leaks are among the most feared, and as we’ve seen, CT with intravenous contrast is a highly sensitive tool for their detection, showing sensitivities between 91-95%. A UGI series, while having a lower sensitivity (around 54%), can still be valuable, especially if marginal radiological evidence of leakage is treated as presumptively positive.
Other complications include staple-line hemorrhage, which often appears as a hematoma on CT. Abscesses, collections of pus, are typically well-visualized on contrast-improved CT as fluid collections with rim improvement. Hernias, particularly internal hernias after Roux-en-Y gastric bypass (RYGB), can cause small bowel obstruction and are best diagnosed with CT, which shows clustered bowel loops or vascular engorgement. Rapid weight loss can also precipitate gallstone formation, making ultrasound a common follow-up imaging modality. Our Gastrointestinal Imaging courses provide a detailed look at these and other abdominal pathologies.
Recommended Imaging Timeline
- Immediate Post-Op (Day 1-2): For procedures involving anastomosis or stapling, a fluoroscopic UGI series is often performed. This is primarily to check for anastomotic leaks and assess the integrity of the new gastric pouch or bypass. While some institutions perform this routinely, others reserve it for symptomatic or high-risk patients.
- Early Complications (First 30 days): If a patient develops symptoms such as persistent abdominal pain, fever, tachycardia, or unexplained fatigue, a CT scan with intravenous contrast is typically requested. This is the go-to modality for suspected leaks, abscesses, or early bowel obstructions.
- 3-6 Months Post-Op: Rapid weight loss increases the risk of gallstone formation. An ultrasound of the gallbladder is often recommended during this period to screen for cholelithiasis, especially if the patient experiences right upper quadrant pain.
- Long-Term Follow-Up: Beyond the initial months, imaging is usually symptom-driven. If a patient experiences weight regain, persistent gastrointestinal issues (like nausea, vomiting, or changes in bowel habits), or new abdominal pain, further imaging (often CT or UGI) may be warranted. Bone density scans (DEXA) are also crucial for long-term monitoring, as bariatric surgery can affect nutrient absorption and bone health. For a comprehensive review of body CT, our Fundamentals of Body CT 5th Ed. is an excellent resource.
Conclusion
Bariatric CT imaging is a continually evolving field, driven by the increasing prevalence of obesity and the rising number of bariatric surgeries. We’ve explored the myriad challenges, from accommodating larger patients on our equipment to mitigating complex artifacts and managing radiation doses effectively. We’ve also highlighted the specific imaging findings characteristic of obese patients and the crucial role of CT in monitoring them, both pre- and post-surgery.
The future of Bariatric CT imaging is bright, with AI and body morphometry promising to revolutionize how we assess risk, predict outcomes, and personalize care for this unique patient population. As radiologic technologists, our commitment to ongoing learning and adaptation is paramount. By embracing advanced techniques and staying informed, we can continue to provide the highest quality diagnostic imaging, ensuring better health outcomes for all our patients, regardless of their size.
For those eager to deepen their expertise and steer the complexities of modern CT imaging, we invite you to Explore our Computed Tomography CE Complete Guide. Your professional development is our priority.
Recent Comments